'Brand new way to treat patients': Ketamine injections approved for Alberta's community facilities
The regulatory body for Alberta doctors has recently updated its regulations allowing non-hospital treatment centres to administer Ketamine to treat serious depression and mental health conditions.
The College of Physicians and Surgeons of Alberta (CPSA) now approves community facilities with in-house anesthesiologists and psychiatrists to offer the dissociative or sedative psychedelic via IV (intravenous).
The Ketatmine-assisted therapy can also be used to manage chronic pain disorders.
"I'm really excited to be on this new frontier, and a brand new way to treat patients," said Dr. Craig Pearce, president of anesthesia for the Alberta Medical Association, and medical director at SABI Mind, a private psychedelic therapy clinic.
Pearce said his best friend died by suicide 27 years ago, and says his work in his new role is driven by a desire to help others who may be experiencing extreme distress.
"If this is an opportunity for me to help rescue and save someone else who has that type of affliction or concern and improve their life, then I'm going to jump at it," said Pearce.
Andrea Daye says she's suffered with depression on and off since she was 16, and underwent Ketamine treatments from June to last August.
"I feel amazing today. Mental health is a journey that goes up and down and zig-zags, but the Ketamine really helped," she said.
Daye said she is no longer an intensive care unit nurse, after suffering from traumatic experiences in a Calgary area hospital during COVID-19 waves in 2021.
She says maintaining her mental health is ongoing, but the therapy helped her find her way out of a major depressive episode last May.
"It is a catalyst and an extremely effective catalyst, more effective than anything I have ever done before," said Daye.
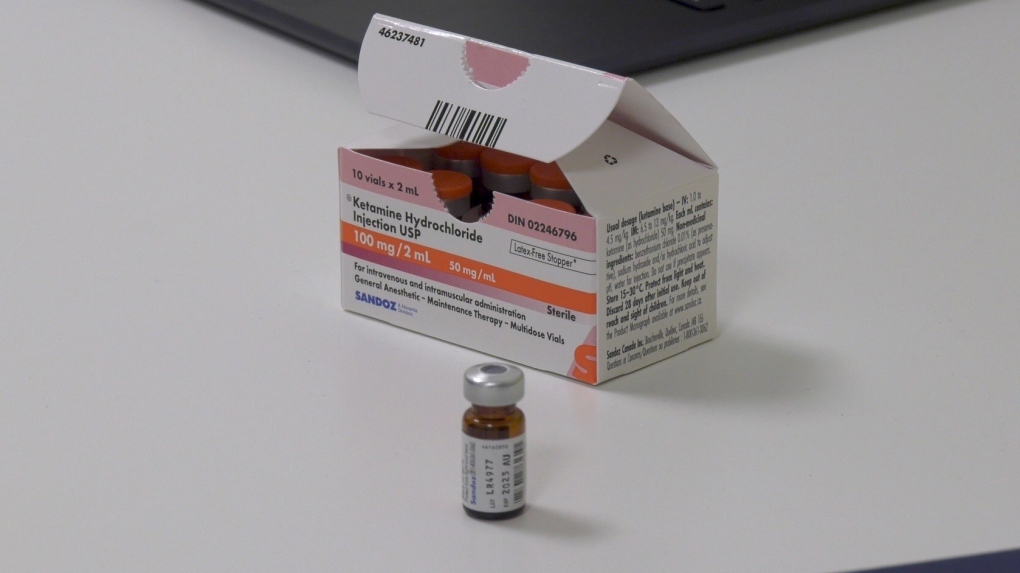
Psychedelic therapy for mood disorders and chronic pain is an emerging field of study, as researchers hope to determine if controlled substances help "treatment-resistant" patients whose conditions don't show improvement with traditional pharmaceuticals or therapies.
"What is it that's really driving these effects? Is it the drugs that are being used or the context in which they're being given? That's what we're really interested in, is really distilling it down to what is the important ingredient that we need to look for," said Dr. Leah Mayo, Parker Psychedelics research chair at University of Calgary.
Mayo says government-funded research will help find answers to questions about the efficacy of psychedelics.
The Centre for Addiction and Mental Health (CAMH) has launched a study through a federal grant to explore how Psilocybin (the chemical in “magic mushrooms") can treat depression and if the hallucinogenic or psychedelic effects are necessary.
"There's a lot that we still don't know about the use of psychedelic drugs and how they actually help people with mental health conditions," said Dr. Ishrat Husain, head of clinical trails at CAMH.
He added, "It may well be in fact that it is the hallucinogenic experience that sort of leads to access to repressed memories and opens up the brain to be more receptive to psychotherapy."
Husain said if the study demonstrates the ingredients can work even without inducing a psychedelic effect it would be easier to put into practise -- saving time, resources and costs.
He says a "trip" can range up to eight hours, and requires medical supervision.
The clinical trial includes 60 adult participants with treatment-resistant depression and will run over a three-year period.
For Dr. Mayo in Calgary, expanded science and research would help provide broader access to effective alternative treatments.
"The people who need these treatments right now, people with really severe mental health conditions might not be able to go to these Ketamine clinics that are available and pay the fees that are associated with it," said Mayo.
At the moment, Ketamine therapy is the only psychedelic approved and regulated in Canada for specific conditions.
There are no therapeutic products containing psilocybin, LSD, MDMA or DMT approved for sale in Canada outside of a clinical trial.
CTVNews.ca Top Stories

BREAKING Celine Dion stages comeback with performance at Paris Olympics opening ceremony
Celine Dion staged the comeback of her career during the opening ceremony at the Olympic Games in Paris.
Jasper wildfire: 'Several weeks' before Jasper can return, premier says
Premier Danielle Smith said Friday afternoon in Hinton while weather conditions are cooler, the Jasper fire is still considered out of control and that Jasper residents can expect to be away from their homes "for several weeks."
Driver charged after flashing high beams at approaching police
Orillia OPP arrested and charged a driver with impaired driving after flashing their high beams.
'He was just gone': Police ramp up search for vulnerable 3-year-old boy in Mississauga, Ont.
Police in Mississauga are conducting a full-scale search of the city’s biggest park for a non-verbal toddler who went missing Thursday evening. Sgt. Jennifer Trimble told reporters Friday morning that there has been no trace of three-year-old Zaid Abdullah since 6:20 p.m., when he was last seen with his parents in Erindale Park, near Dundas Street West and Mississauga Road.
Irish museum pulls Sinead O'Connor waxwork after just one day due to backlash
An Irish museum will withdraw a waxwork of singer-songwriter Sinéad O’Connor just one day after installing it, following a backlash from her family and the public, it told CNN in a statement on Friday.
Turpel-Lafond won't sue CBC over Cree heritage report that took 'heavy toll': lawyer
The lawyer for a former judge whose claims to be Cree were questioned in a CBC investigation says his client is not considering legal action against the broadcaster after the Law Society of British Columbia this week backed her claims of Indigenous heritage.
Health Canada warns some naloxone kits contain false instructions
Health Canada is warning some take-home naloxone kits come with bad instructions that should be ignored in favour of the correct guidance.
Winnipeg senior's account overdrawn for $146,000 water bill
A Winnipeg senior is getting soaked with a six figure water bill.
Paris Olympics kicks off with ambitious but rainy opening ceremony on the Seine River
Celebrating its reputation as a cradle of revolution, Paris kicked off its first Summer Olympics in a century on Friday with a rain-soaked, rule-breaking opening ceremony studded with stars and fantasy along the Seine River.































